Shockwave Therapy Geelong
Radial Shockwave Therapy
We are excited to be to be able to announce Radial Shockwave Therapy is available at our clinic. This technology and treatment method has been shown in research studies to be effective in just 3-6 treatments for chronic tendinopathies of the feet, achilles, knee, shoulder, elbow and hip.
I am a big fan of shockwave therapy for treating all sorts of chronic tendinopathies. In my seventeen years as an osteopath the only thing that would rival it in terms of recovery from pain and incapacity is cortisone. However, unlike cortisone there are very few side effects with shockwave other than the possibility of local bruising. Cortisone on the other hand has a myriad of side effects including tendon rupture, diabetes and bone necrosis.
So what is Shockwave Therapy?
Shockwave (SW) therapy was originally used in the 1980s for the treatment of kidney stones. The process involves breaking down the stones in what is called lithotripsy. It was then found to work well in breaking down boney heel spurs. It was then also found to help with foot pain in the absence of a spur (plantarfasciitis) and from there further studies have targeted a range of chronic tendinopathies at different sites around the body.
We have used SW at our clinic for the last 2 years and have had some great results. One of our patients who hadn’t been able to lift her arm above shoulder level for around 9 months without shoulder pain raised her arm overhead without pain in just her first treatment. She simply could not believe it! Although most people don't have this kind of instant response, we have successfully treated many patients for plantar fasciitis, achilles, hamstring and elbow (golfers and tennis elbow) tendinopathies, as well as shoulder (rotator cuff) tendinopathies.
The beauty of SW is that it increases healing whilst having an analgesic effect. The analgesic effect is thought to be brought about by a depletion of a neurotransmitter of pain called “substance P”. (It is the same neurotransmitter that is broken down by chilli. So if you ever have had your mouth go numb after eating chilli this is the reason).
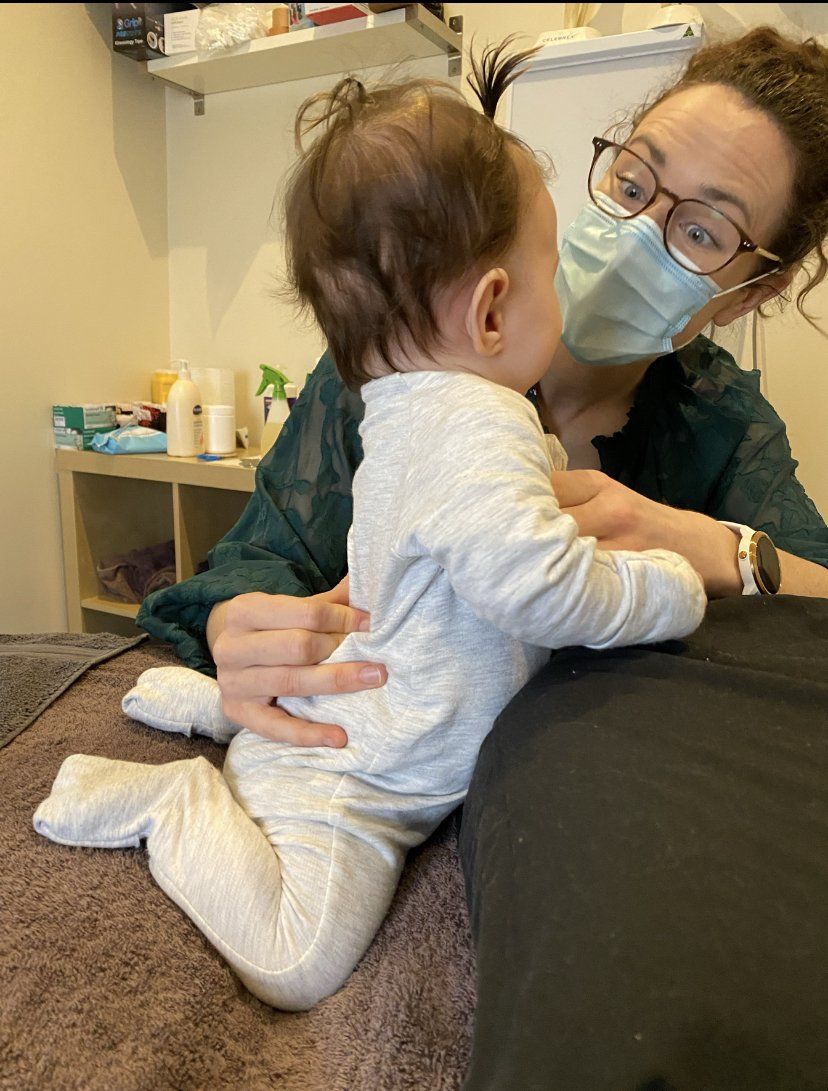
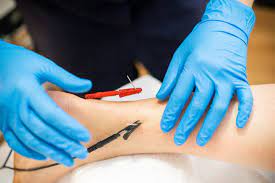
Our SW is conducted by our qualified practitioners. It uses a pneumatically powered hand piece that generates radial shockwaves, which are transmitted to the site of the injury through a conducting gel. The treatment session uses around 2000 pulsed shockwaves into the affected area and takes anywhere from 3-10 minutes. This is usually incorporated into the overall treatment with manual therapy and sometimes post treatment taping.
Most patients will notice some pain relief immediately after therapy, others can take up to 4-5 sessions to achieve significant pain relief. This really depends on the severity and length of your condition. It also depends on how well the painful tissues are targeted. For this reason at the start of the treatment it can be a little painful before the analgesic effect takes place.
Our Swiss Dolorclast SW generator is used in most research articles (see below) and as far as we are concerned this is the best SW generator on the market and is the only SW generator that is FDA approved as a therapeutic device.
Shockwave Therapy can help with the following conditions:
- Jumper’s knee/patella tendinitis
- Frozen shoulder - adhesive capsulitis shoulder (2)
- Calcific tendinitis of the shoulder
- Tennis and Golfers elbow
- Osgood Schlatters disease (3)
- Tennis and Golfers elbow: SW is clinically proven (3) to reduce pain, improve function in patients with tennis elbow and is proven to be as effective as a steroid injection (5).
- Achilles Tendinopathy: SW trials have confirmed excellent results with decreasing pain and increasing achilles function compared with either sham shockwave therapy or exercises in isolation (6).
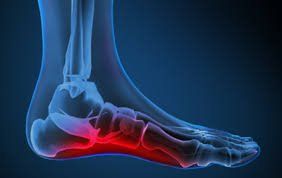
- Plantar Fasciitis and Heel Spurs: In a recent study, the authors looked at the efficacy of eight different types of treatment for plantar fasciitis. It was concluded that SW therapy ranked as the best outcome and is considered the “optimal treatment” (7). Another study showed that combining SW with a practitioner-guided stretching program has been proven to deliver clinically superior outcomes for plantar fasciitis sufferers than other forms of treatment.
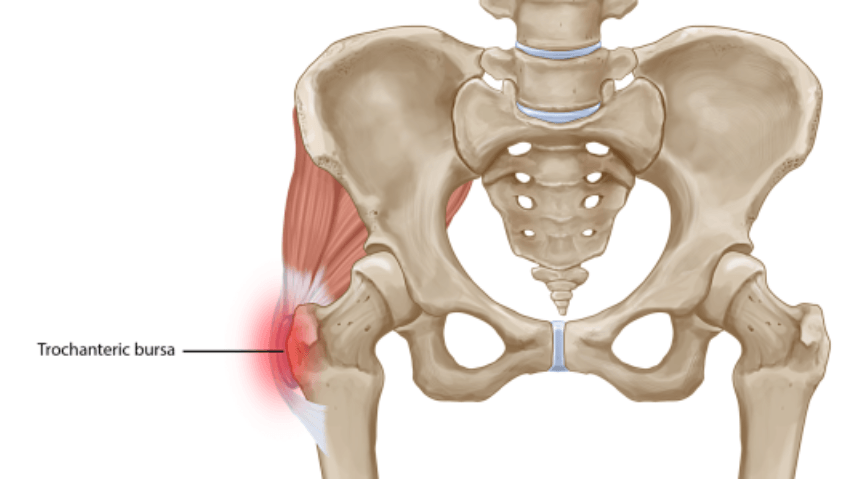
- Hip - Greater Trochanteric Pain Syndrome: A randomised controlled clinical trial of 229 people showed SW was significantly more successful than steroid injection (8).
- Shin Splints - Medial Tibial Stress Syndrome: A clinical trial showed that 40 of 47 shin splint sufferers were able to return to their preferred sport at their pre-injury level after 15 months, versus only 22 in a control group (9).
- Calcifying Tendinopathy of the Shoulder: Clinical trials revealed that SW therapy for calcific tendinitis of the shoulder showed good to excellent results in 87.9% of shoulders treated. Among SW patients, calcium deposits were significantly reduced (10).
What is the cost of shockwave therapy?
The cost of SW therapy is the cost of one of our standard consultations plus a fee depending on how many body parts.
1 body Part $55
2 Body parts $75
3 Body parts $95.
As your shockwave therapy is performed by a qualified practitioner, private health rebates and Medicare (CDM plan) can be utilised towards to cost of the standard consultation part of the treatment.
Will I need a referral for Shockwave therapy?
No you do not need a referral, but you require an initial assessment by one of our qualified practitioners to determine if SW therapy is suitable for you.
So if you have had a tendinopathy for more than several months come and see us and we will see if SW is suitable for you. If SW therapy is not suitable for you, we will guide you towards another suitable treatment or for further investigations.
To reiterate what we have covered, SW is safe, it is effective, it has few side effects and you can get back to your daily activities right away. It’s a walk in and walk out treatment. We are excited to bring this to our clients and we look forward to hearing from all of you chronic tendinopathy suffers out there soon.
Darrell Pummeroy
Principal Osteopath & Director
1. Arch Orthop Trauma Surg. 2010 Nov; 130(11:1343-1347)
2.Int J Prev Med. 2014 Jul; 5(7): 875–881.
3. European j. biomed. pharm. sci, 2015, Volume 2, Issue 2, 78-90.
4. Europia Medicophysica 2005;41:17-25.
5. Annals Rehabilitation Medicine 2012;36(5):681–7.
6. Am J Sports Med (2009) 37(3):463-70.
7. J Cell Physiol. 2018 Aug 4. doi: 10.1002/jcp.26907
8. International Journal of Surgery 24 (2015) 135-42.
9. Am J Sports Medicine (2009); 37:1981-9012. Am J Sports Medicine (2010); 38:125-32
10. J Shoulder Elbow Surg 2008;17:55-9